SUMMARY: Breast cancer is the most common cancer among women in the US and about 1 in 8 women (12%) will develop invasive breast cancer during their lifetime. Approximately 246,660 new cases of invasive breast cancer will be diagnosed in 2016 and 40,450 women will die of the disease. Axillary lymph node evaluation is an important part of breast cancer staging and the presence of axillary lymph metastases decreases the 5-year survival rate by 28-40%. Axillary lymph node status remains the most powerful predictor of breast cancer recurrence and survival. Axillary Lymph Node Dissection (ALND) was first advocated in the 18th century as part of the treatment of invasive breast cancer and has been standard practice until 2 decades back. ALND can be associated with significant morbidities such as upper limb lymphedema, pain, and sensitivity disorders and this can have a major psychological impact on breast cancer patients. Sentinel Lymph Node Biopsy (SLNB) which was introduced into clinical practice in the mid 1990’s, however has now become a standard method of treatment for stage I and II breast cancer. This therapeutic surgical modality facilitates selective histopathological evaluation of the sentinel lymph nodes rather than routine lymphadenectomy, thereby sparing the patient from the morbidities associated with ALND. Several studies have shown no statistically significant difference in the axillary recurrence risk and survival rates, between these two therapeutic surgical modalities.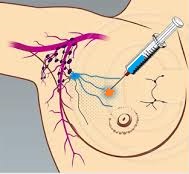
Neoadjuvant chemotherapy is considered standard practice in women with locally advanced breast cancer. This intervention increases the possibility of breast conserving surgery in women with locally advanced breast cancer and for tumors more than 3 cm in diameter, with good cosmetic outcomes. Close to half of the patients treated with neoadjuvant chemotherapy have no axillary lymph node involvement at the time of surgery. GANEA 2 trial was conducted to assess the feasibility and safety of SLNB, a less invasive procedure, for patients treated with neoadjuvant chemotherapy.
The researchers enrolled 590 patients with large, operable breast tumors who had no cancer in the lymph nodes as determined by axillary sonography with fine needle cytology. All patients received neoadjuvant chemotherapy, and then underwent surgery and Sentinel Lymph Node Biopsy. Cancer cells were detected in the Sentinel Lymph Node Biopsy specimens of 139 patients and these patients underwent Axillary Lymph Node Dissection.
No cancer cells were detected in the Sentinel Lymph Node Biopsy samples from 432 patients. Follow-up data was available for 416 of these patients. The median follow-up was 35.8 months. The Disease Free Survival at 3 years in the patient group who had no cancer cells in the Sentinel Lymph Node Biopsy sample, and therefore did not receive Axillary Lymph Node Dissection, was 94.8%. The Overall Survival rate was 98.7%.
The authors concluded that Axillary Lymph Node Dissection could be avoided in patients who have no signs of cancer involvement in the axillary lymph nodes, based on sonographic axillary assessment, prior to neoadjuvant chemotherapy and Sentinel Lymph Node Biopsy findings after neoadjuvant chemotherapy. In this study, the Disease Free Survival and Overall Survival rates for the patients who underwent only a Sentinel Lymph Node Biopsy after neoadjuvant chemotherapy, were comparable with the historical survival rates for patients in this situation who had Axillary Lymph Node Dissection rather than Sentinel Lymph Node Biopsy. Classe JM, Loaec C, Alran S, et al. Sentinel node detection after neoadjuvant chemotherapy in patient without previous axillary node involvement (GANEA 2 trial): follow-up of a prospective multi-institutional cohort. Presented at: 2016 San Antonio Breast Cancer Symposium; December 6-10, 2016; San Antonio, TX. Abstract S2-07.

