SUMMARY: The American Cancer Society estimates that about 28,000 new cases of stomach cancer will be diagnosed in the United States for 2017 and about 10,960 people will die of this disease. It is a leading cause of cancer-related deaths in the world. Patients with operable Gastric or GastroEsophageal adenocarcinoma frequently receive perioperative or neoadjuvant chemotherapy prior to surgical resection, as this has been associated with a modest improvement in Overall Survival (OS), compared with surgery alone. However, approximately 50% of the patients undergoing surgical resection will die of recurrent disease. Further perioperative chemotherapy can be associated with significant toxicities. For patients with GastroEsophageal cancer receiving neoadjuvant treatment, there are presently no validated prognostic biomarkers, and patient selection is based on preoperative clinical staging.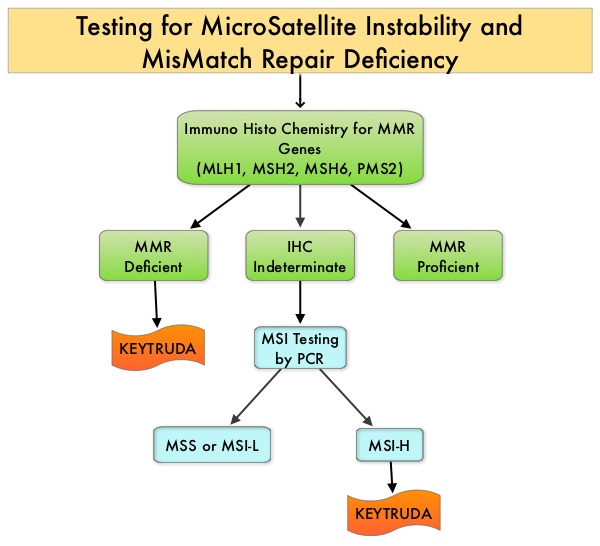
The DNA MisMatchRepair (MMR) system is responsible for molecular surveillance and works as an editing tool that identifies errors within the microsatellite regions of DNA and removes them. Defective MMR system leads to MSI (Micro Satellite Instability) and hypermutation, triggering an enhanced antitumor immune response. MSI (Micro Satellite Instability) is therefore a hallmark of defective/deficient DNA MisMatchRepair (MMR) system and occurs in 15% of all colorectal cancers. Defective MisMatchRepair can be a sporadic or heritable event. Approximately 65% of the MSI colon tumors are sporadic and when sporadic, the DNA MisMatchRepair gene is MLH1. Defective MisMatchRepair can also manifest as a germline mutation occurring in 1 of the 4 MisMatchRepair genes which include MLH1, MSH2, MSH6, PMS2. This produces Lynch Syndrome (Hereditary Nonpolyposis ColoRectal Carcinoma – HNPCC), an autosomal dominant disorder and is the most common form of hereditary colon cancer, accounting for 35% of the MSI colorectal cancers. MSI tumors tend to have better outcomes and this has been attributed to the abundance of Tumor Infiltrating Lymphocytes in these tumors, from increased immunogenicity. These tumors are susceptible to PD-1 blockade and respond to treatment with checkpoint inhibitors such as KEYTRUDA® (N Engl J Med 372:2509-2520, 2015). Other MSI-High and dMMR (MMR deficient) tumors include, Endometrial and GastroIntestinal tumors and to a lesser extent Breast, Prostate, Bladder and Thyroid tumors.
MSI (Micro Satellite Instability) testing is performed using a PCR based assay and MSI-High refers to instability at 2 or more of the 5 mononucleotide repeat markers and MSI-Low refers to instability at 1 of the 5 markers. Patients are considered Micro Satellite Stable (MSS) if no instability occurs. MSI-L and MSS are grouped together because MSI-L tumors are uncommon and behave similar to MSS tumors. Tumors considered MSI-H have deficiency of one or more of the DNA MisMatchRepair genes. MMR gene deficiency can be detected by ImmunoHistoChemistry (IHC). MLH1 gene is often lost in association with PMS2. Approximately 10-20% of Gastric cancers are MSI high or MMR Deficient. Several retrospective studies have suggested favorable outcomes in patients with Gastric cancer with high MSI tumors, although none of these studies had a control group.
In the MAGIC trial (The UK Medical Research Council Adjuvant Gastric Infusional Chemotherapy), which is an open-label, multicenter, phase III study, patients with resectable GastroEsophageal cancer were randomized to receive either 6 cycles of perioperative Epirubicin, Cisplatin, and Infusional 5-FU (3 cycles before and 3 cycles after resection) plus surgery, or undergo surgery alone. In this study, patients treated with perioperative chemotherapy had improved Overall Survival (OS) compared with patients treated with surgery alone (5-year OS 36% versus 23%; HR=0.75; P=0.009).
The authors in this study additionally evaluated patients with operable GastroEsophageal cancers with High MicroSatellite Instability (MSI-H) or MMR deficiency (dMMR), and compared their survival with patients who had MicroSatellite Stable (MSS) GastroEsophageal cancer, when these patients were treated with surgery alone or surgery plus perioperative chemotherapy. The authors thus assessed survival outcomes based on MSI/MMR deficiency. Of the 503 clinical trial participants, MSI results were available for 303 patients and both MSI and MMR results were available in 254 patients. Patients who had High MSI or MMR deficiency treated with surgery alone, had a median OS that was Not Reached (NR) compared with a median Overall Survival (OS) of 20.5 months, among those who had neither high MSI nor MMR deficiency (HR=0.42; P=0.09). In contrast, patients who had either a High MSI or MMR deficiency, treated with surgery plus perioperative chemotherapy had a median OS of 9.6 months compared with a median OS of 19.5 months, among those who had neither High MSI nor MMR deficiency (HR=2.18; P=0.03). The overall concordance rate between MSI-H and MMR deficient status was 97.6%.
Based on these findings the authors concluded that patients with operable GastroEsophageal cancer with High MicroSatellite Instability or MMR deficiency, did not benefit from perioperative chemotherapy and could be spared from the toxicities of chemotherapy. These patients may benefit from therapy with PD-1 inhibitors, although this will need to be further investigated. If independently validated, MSI or MMR deficiency, determined by preoperative biopsies, could be used to select patients for perioperative chemotherapy. Mismatch Repair Deficiency, Microsatellite Instability, and Survival. An Exploratory Analysis of the Medical Research Council Adjuvant Gastric Infusional Chemotherapy (MAGIC) Trial. Smyth EC, Wotherspoon A, Peckitt C, et al. JAMA Oncol. 2017;3:1197-1203.

