The ACS recently updated Colorectal Cancer Screening Guideline using prevailing evidence as well as microsimulation modeling analyses. The new guideline does not prioritize among screening test options. This is because test preferences vary among individuals and the guidelines development committee emphasized that screening rates could be improved by endorsing the full range of tests without preference. Adults born around 1990 have twice the risk of colon cancer and four times the risk of rectal cancer compared with adults born around 1950, who have the lowest risk. In the updated guideline, screening is recommended earlier, starting at age 45 years and may be performed with either a high-sensitivity stool-based test or a structural (visual) exam, depending on patient preference and test availability.
Tag: Colon Cancer
American Cancer Society Updates Colorectal Cancer Screening Guideline for Average Risk Adults
SUMMARY: The American Cancer Society estimates that approximately 140,250 new cases of ColoRectal Cancer will be diagnosed in the United States in 2018 and about 50,630 patients are expected to die of the disease. The lifetime risk of developing CRC is about 1 in 21 (4.7%). ColoRectal cancer (CRC) is the fourth most common cancer diagnosed among adults in the US and the second leading cause of death from cancer.
The ACS recently updated Colorectal Cancer Screening Guideline using prevailing evidence as well as microsimulation modeling analyses, and included a new evaluation of the age, to begin screening by race and sex and additional modeling that incorporates changes in United States CRC incidence. The ACS Guideline Development Group applied the Grades of Recommendations, Assessment, Development, and Evaluation (GRADE) criteria in developing and rating the recommendations. The new guideline does not prioritize among screening test options. This is because test preferences vary among individuals and the guidelines development committee emphasized that screening rates could be improved by endorsing the full range of tests without preference.
Even though the incidence of Colorectal cancer (CRC) in the United States has been rapidly declining overall in people 55 and over primarily driven by screening, among adults younger than 55 years there was a 51% increase in the incidence of colorectal cancer (CRC) from 1994 to 2014 and a 11% increase in deaths from 2005 to 2015. Adults born around 1990 have twice the risk of colon cancer and four times the risk of rectal cancer compared with adults born around 1950, who have the lowest risk. Studies suggest that the younger individuals will continue to be at a higher risk as they age. The increase in the incidence of CRC in young adults has been attributed to western life style including high carbohydrate, high fat, low fiber diet which can initiate inflammation and proliferation in the colonic mucosa within two weeks. Other lifestyle factors associated with CRC include obesity, high consumption of processed meat and alcohol, low levels of physical activity and cigarette smoking. Further, young patients are 58% more likely than older patients to be diagnosed with advanced versus localized stage CRC, due to delayed follow up of symptoms, sometimes for years, and these young adults are less likely to be screened for colon cancer, despite their symptoms.
The current ACS recommendations are as follows:
1) Adults aged 45 and older with an average risk of colorectal cancer should undergo regular screening with either a high-sensitivity stool-based test or a structural (visual) exam, depending on patient preference and test availability.
2) As a part of the screening process, all positive results on non-colonoscopy screening tests should be followed up with timely colonoscopy.
3) The recommendation to begin screening at age 45 years is a “qualified recommendation”. The change in starting age is designated as a “qualified recommendation” because there is less direct evidence of the balance of benefits and harms, or patients’ values and preferences, related to colorectal cancer screening in adults aged 45 to 49, since most studies have only included adults aged 50 and older.
4) The recommendation for regular screening in adults aged 50 years and older is designated as a “strong recommendation,” on the basis of the greater strength of the evidence and the judgment of the overall benefit.
5) Average-risk adults in good health with a life expectancy of greater than 10 years should continue colorectal cancer screening through age 75 years.
6) Clinicians should individualize colorectal cancer screening decisions for individuals aged 76 through 85 years, based on patient preferences, life expectancy, health status, and prior screening history.
7) Clinicians should discourage individuals over age 85 years from continuing colorectal cancer screening.
Test options for CRC screening include the following:
Stool-based tests
1) Highly sensitive Fecal Immunochemical Test (FIT) annually
2) Highly sensitive guaiac-based Fecal Occult Blood Test (gFOBT) annually
3) Multi-targeted stool DNA test every 3 years
Visual exams
1) Colonoscopy every 10 years
2) CT colonography (virtual colonoscopy) every 5 years
3) Flexible sigmoidoscopy every 5 years
Colorectal cancer screening for average-risk adults: 2018 guideline update from the American Cancer Society. Wolf AM, Fontham ET, Church TR, et al. CA Cancer J Clin 2018;68:250-281.
YERVOY® and OPDIVO®
The FDA on July 10, 2018 granted accelerated approval to YERVOY® (Ipilimumab), for use in combination with OPDIVO® (Nivolumab), for the treatment of patients 12 years of age and older with MicroSatellite Instability-High (MSI-H) or MisMatch Repair deficient (dMMR) metastatic Colorectal Cancer (mCRC), that has progressed following treatment with a Fluoropyrimidine, Oxaliplatin, and Irinotecan. YERVOY® and OPDIVO® are products of Bristol-Myers Squibb Company Inc.
FDA Approves OPDIVO® and YERVOY® Combination for Metastatic Colorectal Cancer
SUMMARY: The FDA on July 10, 2018, granted accelerated approval to YERVOY® (Ipilimumab) for use in combination with OPDIVO® (Nivolumab), for the treatment of patients 12 years of age and older with MicroSatellite Instability-High (MSI-H) or MisMatch Repair deficient (dMMR) metastatic ColoRectal Cancer, that has progressed following treatment with a Fluoropyrimidine, Oxaliplatin, and Irinotecan. The FDA in July, 2017, granted accelerated approval to single agent OPDIVO® (Nivolumab) for treatment of this same group of patients. ColoRectal Cancer (CRC) is the third most common cancer diagnosed in both men and women in the United States. The American Cancer Society estimates that approximately 140,250 new cases of CRC will be diagnosed in the United States in 2018 and about 50,630 patients are expected to die of the disease. The lifetime risk of developing CRC is about 1 in 21 (4.7%).
The DNA MisMatchRepair (MMR) system is responsible for molecular surveillance and works as an editing tool that identifies errors within the microsatellite regions of DNA and removes them. Defective MMR system leads to MSI (Micro Satellite Instability) and hypermutation, triggering an enhanced antitumor immune response. MSI (Micro Satellite Instability) is therefore a hallmark of defective/deficient DNA MisMatchRepair (dMMR) system and occurs in 15% of all colorectal cancers. Defective MisMatchRepair can be a sporadic or heritable event. Approximately 65% of the MSI tumors are sporadic and when sporadic, the DNA MisMatchRepair gene is MLH1. Defective MisMatchRepair can also manifest as a germline mutation occurring in 1 of the 4 MisMatchRepair genes which include MLH1, MSH2, MSH6, PMS2. This produces Lynch Syndrome (Hereditary Nonpolyposis Colorectal Carcinoma – HNPCC), an Autosomal Dominant disorder and is the most common form of hereditary colon cancer, accounting for 35% of the MSI colorectal cancers. MSI tumors tend to have better outcomes and this has been attributed to the abundance of tumor infiltrating lymphocytes in these tumors from increase immunogenicity. These tumors therefore are susceptible to blockade with immune checkpoint inhibitors. MSI (Micro Satellite Instability) testing is performed using a PCR based assay and MSI-High refers to instability at 2 or more of the 5 mononucleotide repeat markers and MSI-Low refers to instability at 1 of the 5 markers. Patients are considered Micro Satellite Stable (MSS) if no instability occurs. MSI-L and MSS are grouped together because MSI-L tumors are uncommon and behave similar to MSS tumors. Tumors considered MSI-H have deficiency of one or more of the DNA MisMatchRepair genes. MMR gene deficiency can be detected by ImmunoHistoChemistry (IHC). MLH1 gene is often lost in association with PMS2. NCCN Guidelines recommend MMR or MSI testing for all patients with a history of Colon or Rectal cancer.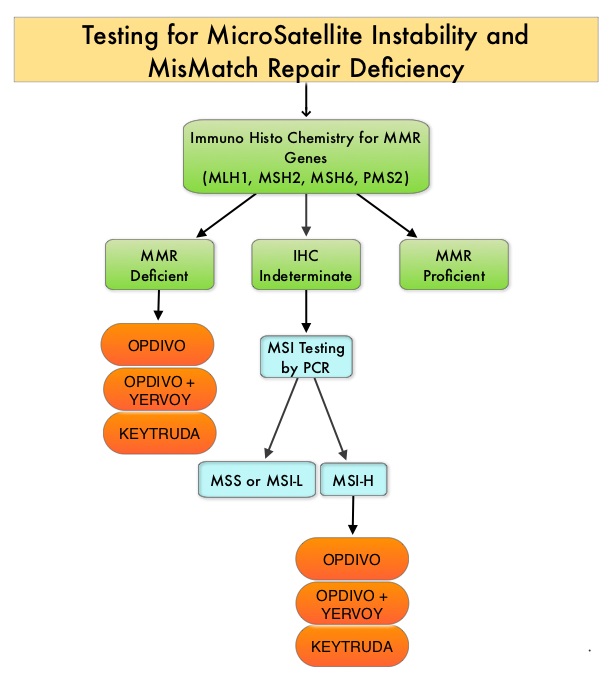
OPDIVO® is a fully human, immunoglobulin G4 monoclonal antibody that binds to the PD-1 receptor and blocks its interaction with PD-L1 and PD-L2, whereas YERVOY® is a fully human immunoglobulin G1 monoclonal antibody that blocks Immune checkpoint protein/receptor CTLA-4 (Cytotoxic T-Lymphocyte Antigen 4, also known as CD152). Blocking the Immune checkpoint proteins unleashes the T cells, resulting in T cell proliferation, activation and a therapeutic response.
This new FDA approval was based on data from the ongoing CheckMate-142, which is a multicenter, open-label, phase II trial, designed to determine within the dMMR/MSI-H population, whether OPDIVO® alone or in combination with another checkpoint inhibitor YERVOY®, could result in meaningful responses in patients with metastatic CRC, following at least one prior line of therapy. This study was not designed to compare the outcomes in cohorts receiving single agent OPDIVO® and combination checkpoint inhibitors. The rationale behind combining OPDIVO® a PD-1 inhibitor and YERVOY®, a CTLA-4 inhibitor, was based on the synergy between these two agents, to promote T-cell antitumor activity, thereby improving upon single-agent activity of OPDIVO®.
This study enrolled 74 patients, who received single agent OPDIVO® 3 mg/kg IV every 2 weeks and 119 patients who received OPDIVO® 3 mg/kg IV plus YERVOY® 1 mg/kg IV, every 3 weeks for four doses, followed by OPDIVO® 3 mg/kg as a single agent every 2 weeks, until unacceptable toxicity or radiographic progression. In this study, from a cohort of 119 patients with MSI-H or dMMR mCRC, 82 patients received prior treatment with a Fluoropyrimidine, Oxaliplatin, and Irinotecan. Among the cohort of 119 patients receiving OPDIVO® plus YERVOY®, the median age was 58 years, 29% had a known history of Lynch syndrome, 24% had BRAF mutations, 37% had KRAS mutations and 22% of patients had high PD-L1 expression (1% or more) on tumor cells at baseline. Primary tumor location was in the right colon in 55% of patients, 25% had left and sigmoid colon disease and 13% had primary tumor in the transverse colon. Seventy six percent (76%) of patients had two or more prior lines of therapy. The Primary end point was investigator-assessed ORR (Overall Response Rate) and Secondary end points included DCR (Disease Control Rate – CR, PR, or stable disease) Safety and tolerability, PFS (Progression Free Survival) and OS (Overall Survival).
At median follow-up of 13.4 months, the ORR in those patients receiving OPDIVO® plus YERVOY®, was 55% and the Disease Control Rate for 12 or more weeks was 80%. Median duration of response was not reached and 94% of the responses were ongoing at data cutoff. PFS and OS rates at 1 year were 71% and 85%, respectively. Further, clinically meaningful and statistically significant improvements were observed in patient-reported outcomes, including functioning, symptoms, and quality of life. Approximately 13% of patients who discontinued treatment because of toxicities still had an ORR of 63%, consistent with that of the overall population. Grade 3 to 4 toxicities occurred in 32% of patients and were manageable. Indirect comparisons in this nonrandomized CheckMate-142 trial suggested that OPDIVO® plus YERVOY® provided numerically higher response rates and improved long term clinical benefit relative to OPDIVO® monotherapy.
It was concluded that OPDIVO® plus YERVOY® results in a high response rates, encouraging PFS and OS at 12 months, with manageable toxicities. These data from the CheckMate-142 study support the use of OPDIVO® as a single agent or in combination with YERVOY®, for the treatment of patients with previously treated dMMR/MSI-H metastatic CRC. Durable Clinical Benefit With Nivolumab Plus Ipilimumab in DNA Mismatch Repair–Deficient/Microsatellite Instability–High Metastatic Colorectal Cancer. Overman MJ, Lonardi S, Wong KYM, et al. J Clin Oncol. 2018;36:773-779
Higher Plasma Vitamin D Levels Associated with Lower Colorectal Cancer Risk
SUMMARY: ColoRectal Cancer (CRC) is the third most common cancer and third leading cause of cancer-related deaths in both men and women in the United States. The American Cancer Society estimates that approximately 140,250 new cases of ColoRectal Cancer will be diagnosed in the United States in 2018 and over 50,630 patients are expected to die of the disease. The lifetime risk of colorectal cancer is 4.2% (1 in 24) in women and 4.5% (1 in 22) in men.
Vitamin D is known for its role in maintaining bone health and there is a growing body of evidence suggesting that Vitamin D has colon cancer preventing properties and may induce antitumor immunity. A study by Song and colleagues (Gut. 2015;64:260-271) showed that high plasma level 25-Hydroxy Vitamin D [25(OH)D] was associated with lower risk of colorectal cancer with intense immune reaction, supporting that vitamin D through tumor-host interaction may play a role in cancer immunoprevention. There also appears to be a strong association between plasma 25(OH)D level and colorectal cancer (CRC) specific mortality, with better outcomes in CRC patients with higher plasma levels of 25(OH)D, treated with a combination of chemotherapy and biologic agents. However the plasma concentrations of 25(OH)D that minimize colorectal cancer risk are unknown and even though epidemiological studies suggest a protective role for vitamin D in colorectal carcinogenesis, the evidence has been inconclusive. The current recommendations regarding vitamin D intake are based only on bone health. Sources of vitamin D include fatty fish like salmon, tuna and mackerel, foods fortified with vitamin D like some dairy products, cereals and orange juice as well as egg yolks. It is recommended that vitamin D be obtained through diet whenever possible rather than sun exposure, because of the risk of skin cancer with excessive UV radiation.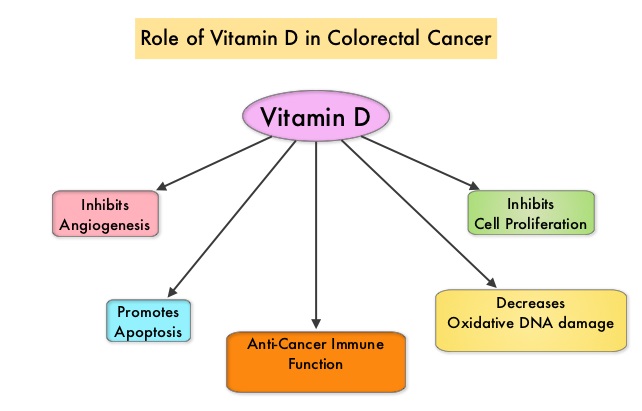
The Institute of Medicine defines vitamin D deficiency as plasma 25(OH)D level of less than 50 nmol/L and the plasma 25(OH)D threshold for fracture prevention is 75 nmol/L. All adults aged 50-70 years and more than 70 years will require at least 600 and 800 IU (15-20 μg) of vitamin D3 per day, respectively, for optimal bone health and muscle function. However, to raise the plasma level of 25(OH)D above 75 nmol/L, individuals will require at least 1500-2000 IU (37.5–50 μg) per day of supplemental vitamin D. Doses of up to 10 000 IU (250 μg) per day have been proven to be safe.
This present study was conducted to address inconsistencies in prior studies, on the protective role for vitamin D in colorectal cancer, and to investigate associations in population subgroups. The authors analyzed participant-level data, collected before colorectal cancer diagnosis, from 17 prospective cohorts which included 5706 colorectal cancer cases and 7107 control participants, from the US, Europe, and Asia, with a wide range of plasma 25(OH)D concentrations. A single, widely accepted assay and laboratory was used for new plasma 25(OH)D measurements, and calibration of previously measured plasma 25(OH)D. This calibration approach enabled the authors to systematically explore risk, utilizing the same assay, over the broad range of vitamin D levels seen internationally.
It was noted that compared to participants with plasma 25(OH)D concentrations sufficient for bone health (50-62.5 nmol/L), those with deficient 25(OH)D levels (less than 30 nmol/L) had a 31% higher risk of colorectal cancer during follow-up, which averaged 5.5 years. In contrast, individuals with plasma 25(OH)D levels above sufficiency for bone health, (75 to less than 87.5 nmol/L) had 19% lower risk and among those with plasma 25(OH)D levels 87.5 to less than 100 nmol/L, the risk of developing colorectal cancer was even lower at 27%. The risk however, did not continue to decline at plasma 25(OH)D levels of 100 nmol/L or greater. The protective association of high levels of plasma 25(OH)D persisted even after adjusting for known colorectal cancer risk factors such as Body Mass Index, physical activity, and other risk factors, and was seen in all subgroups examined. The protective association was more significant in women than men at plasma 25(OH)D levels above bone health sufficiency. For each 25 nmol/L increment in plasma 25(OH)D levels, colorectal cancer risk was 19% lower in women and 7% lower in men.
It was concluded that higher plasma 25(OH)D levels (75-100 nmol/L) was associated with a statistically significant lower colorectal cancer risk in women and non-statistically significant lower risk in men. This study suggested that the optimal plasma 25(OH)D level concentrations for colorectal cancer risk reduction appear higher than the levels recommended for bone health. Circulating Vitamin D and Colorectal Cancer Risk: An International Pooling Project of 17 Cohorts. McCullough ML, Zoltick ES, Weinstein SJ, et al. JNCI: Journal of the National Cancer Institute, https://doi.org/10.1093/jnci/djy087. Published: 14 June 2018.
Elevated Postoperative CEA is an Early Indicator of Colon Cancer Recurrence
SUMMARY: ColoRectal Cancer (CRC) is the third most common cancer diagnosed in both men and women in the United States. The American Cancer Society estimates that approximately 140,250 new cases of ColoRectal Cancer will be diagnosed in the United States in 2018 and over 50,630 patients are expected to die of the disease. CarcinoEmbryonic Antigen (CEA) is a group of highly related glycoproteins involved in cell adhesion and was first described in 1965. CEA is normally produced in gastrointestinal tissue during fetal development and is usually present at very low levels in the serum of healthy adults. Elevated serum levels of CEA are seen in certain malignancies and also in heavy smokers. Measurement of CEA is recommended for patients with colorectal cancer as a surveillance tool for early detection of potentially curable recurrent disease, following primary resection. Further, elevated preoperative CEA in patients with nonmetastatic colorectal cancer is associated with worse outcomes, in patients with early-stage disease (Stages I-III), independent of tumor stage. Lack of CEA normalization after resection of the primary tumor, is indicative of residual occult disease. Clinically, patients with an elevated preoperative CEA and an otherwise normal contrast-enhanced CT of the chest, abdomen, and pelvis proceed to surgery with the assumption that the primary lesion is the source of the elevated CEA.
This study was conducted to determine whether pre or postoperative CEA is more prognostic and more specifically whether patients with elevated preoperative CEA that normalizes after resection of the primary tumor had a risk of recurrence similar to that of patients with normal preoperative CEA. In this retrospective cohort study conducted at a comprehensive cancer center, 1027 consecutive patients with Stage I-III colon cancer who underwent curative resection and who had a preoperative CEA result available, were identified. Patients were then grouped into 3 cohorts – normal preoperative CEA, elevated preoperative but normalized postoperative CEA, and elevated preoperative and postoperative CEA. The Primary end point was Recurrence Free Survival (RFS) at 3 years.
The 3-year RFS rate for the patients with elevated preoperative CEA (N=312) was 82.3% compared with 89.7% for the patients (N=715) with normal preoperative CEA (HR=1.68; P=0.05). This represented a 7.4% higher 3-year RFS among patients with normal preoperative CEA compared with those with elevated preoperative levels. The negative prognostic impact of elevated preoperative CEA was negated in those patients whose CEA normalized in the postoperative period. Patients with elevated postoperative CEA (N=57) had a 3-year RFS of 74.5% compared with 89.4% for the patients with either normal preoperative CEA (N=715) or normalized postoperative CEA (N=142), (HR=2.53; P=0.001). This represented a 14.9% higher 3-year RFS for patients with normal postoperative CEA, regardless of preoperative level, compared to those with elevated postoperative CEA. Multivariate analyses confirmed that elevated postoperative CEA but not normalized postoperative CEA was independently associated with shorter RFS.
It was concluded that elevated preoperative CEA that normalizes after resection is not an indicator of poor prognosis. Patients with elevated postoperative CEA are at increased risk for recurrence especially within the first 12 months after surgery. Routine measurement of postoperative, rather than preoperative CEA is strongly recommended and CEA can be a valuable biomarker and is an early indicator of tumor recurrence. Association of Preoperative and Postoperative Serum Carcinoembryonic Antigen and Colon Cancer Outcome. Konishi T, Shimada Y, Hsu M, et al. JAMA Oncol. 2018;4:309-315
Shorter Duration of Adjuvant Chemotherapy for Stage III Colon Cancer
SUMMARY: ColoRectal Cancer (CRC) is the third most common cancer diagnosed in both men and women in the United States. The American Cancer Society estimates that approximately 140,250 new cases of ColoRectal Cancer will be diagnosed in the United States in 2018 and over 50,630 patients are expected to die of the disease. Adjuvant chemotherapy for patients with resected, locally advanced, node-positive (stage III) colon cancer, has been the standard of care since the 1990s. Adjuvant treatment with an ELOXATIN® (Oxaliplatin) based chemotherapy regimen has been considered standard intervention since 2004, for patients with stage III colon cancer, following surgical resection, and has been proven to decrease the chance of recurrent disease. Chemotherapy regimens have included (FOLFOX – Leucovorin, 5-FluoroUracil, ELOXATIN®) or CAPOX/XELOX (XELODA®/Capecitabine and ELOXATIN®), given over a period of 6 months. ELOXATIN® can however be associated with neuropathy which can be long lasting or permanent, depending on the duration of therapy. Additional toxicities with longer duration of chemotherapy include diarrhea, fatigue as well as more office visits.
The IDEA Collaboration is a prospective, pre-planned pooled analysis of 6 concurrently conducted randomized phase III trials, which included 12,834 patients from 12 countries. The goal of this study was to determine if 3 months of adjuvant chemotherapy would be as effective as 6 months of therapy and would be non-inferior. Of the enrolled patients with stage III disease, 13% had T1-2 disease, 66% had T3 tumors and 21% had T4 tumors. Seventy one percent (71%) had N1 disease and 28% of the patients had N2 disease. Approximately 60% had low-risk disease (T1-3, N1) and 40% had high-risk (T4 or N2). Overall, about 40% of patients received CAPOX regimen and 60% received FOLFOX regimen. The primary endpoint was Disease Free Survival (DFS).
At a median follow up of 41.8 months, although non-inferiority of 3 months of therapy as compared with 6 months of therapy could not be confirmed in the overall treatment population, clinically relevant findings according to treatment were noted, in prespecified subgroups of patients. Among those patients who received FOLFOX regimen, 6 months of adjuvant therapy was superior to 3 months (HR=1.16; P=0.001 for superiority of 6-month therapy). However, among those patients who received CAPOX, the Disease Free Survival for 3 months versus 6 months was non-inferior (HR=0.95; P=0.006), and this was highly significant.
In an exploratory analysis, it was noted that among the patient group with low-risk cancers (T1-3, N1 cancers), 3 months of therapy was non-inferior to 6 months of therapy (HR= 1.01) with 3-year disease-free survival of 83.1% and 83.3%, respectively. However, among the patients with high-risk cancers (T4, N2, or both), 6 months of adjuvant therapy was superior to 3 months (HR= 1.12; P=0.01 for superiority).
When subgroup analysis was performed according to treatment and risk group, among the patients with low-risk tumors, 3 months of adjuvant therapy with CAPOX was non-inferior to 6 months of therapy. Outcomes after 3 months of adjuvant FOLFOX therapy were worse than those after 6 months, independent of risk group. For patients with high-risk tumors, 6 months of adjuvant therapy with FOLFOX was superior to 3 months, with a 3-year disease-free survival of 64.7% versus 61.5%. It has been hypothesized that the protracted delivery of a Fluoropyrimidine with CAPOX might have been more effective than the twice-monthly 5-FUinfusions with FOLFOX as an adjuvant therapy. Grade 2 or more neurotoxicity was significantly lower for patients who received 3 months of adjuvant therapy versus 6 months (P <0.0001), regardless of the treatment regimen (17% vs 48% for FOLFOX and 15% vs 45% for CAPOX/XELOX, respectively).
It was concluded by the IDEA collaboration that, a risk-based approach has to be taken when making adjuvant chemotherapy recommendations for patients with stage III colon cancer, taking into consideration choice of treatment regimen and duration of therapy. In patients treated with adjuvant CAPOX/XELOX regimen, 3 months of therapy was as effective as 6 months, particularly in the low risk subgroup. In patients treated with FOLFOX, 6 months of adjuvant therapy compared to 3 months, resulted in a higher rate of Disease Free Survival, particularly in the high-risk subgroup. Duration of Adjuvant Chemotherapy for Stage III Colon Cancer. Grothey A, Sobrero AF, Shields AF, et al. N Engl J Med 2018; 378:1177-1188
Treatment Sequencing with STIVARGA® before ERBITUX® Improves Survival in Metastatic Colorectal Cancer
SUMMARY: ColoRectal Cancer (CRC) is the third most common cancer diagnosed in both men and women in the United States. The American Cancer Society estimates that approximately 140,250 new cases of CRC will be diagnosed in the United States in 2018 and about 50,630 patients are expected to die of the disease. The lifetime risk of developing CRC is about 1 in 21 (4.7%). Even though colon cancer localized to the bowel is potentially curable with surgery and adjuvant chemotherapy, advanced colon cancer is often incurable. Standard chemotherapy when combined with anti EGFR (Epidermal Growth Factor Receptor) targeted monoclonal antibodies such as VECTIBIX® (Panitumumab) and ERBITUX® (Cetuximab) as well as anti VEGF agent AVASTIN® (Bevacizumab), have demonstrated improvement in Progression Free Survival (PFS) and Overall Survival (OS). The benefit with anti EGFR agents however is only demonstrable in patients with metastatic CRC, whose tumors do not harbor KRAS mutations in codons 12 and 13 of exon 2 (KRAS Wild Type). It is now also clear that even among the KRAS Wild Type patients, about 15-20% have other rare mutations such as NRAS and BRAF mutations, which confer resistance to anti EGFR agents. Therefore, pan RAS (expanded RAS) testing is now recommended.
STIVARGA® (Regorafenib), is an oral multi-kinase inhibitor approved by the FDA for the treatment of patients with metastatic CRC, who have progressed on 5FU, ELOXATIN® (Oxaliplatin), CAMPTOSAR® (Irinotecan), anti-VEGF and anti-EGFR therapies. STIVARGA® inhibits multiple kinases including VEGF1, VEGF2, VEGF3, PDGFR, FGFR involved in tumor angiogenesis and KIT, RET, RAF-1, BRAF involved in oncogenesis. The approval was based on a phase III trial in which patients receiving STIVARGA® had a statistically significant improvement in the Overall Survival and Progression Free Survival, compared to placebo.
Both STIVARGA® and ERBITUX® are approved for metastatic CRC. The optimal sequencing of these drugs however, has remained unclear. The current standard of care is to offer an ERBITUX® based regimen followed by STIVARGA®. STIVARGA® however has demonstrated activity in patients with metastatic CRC, when given earlier in the course of the disease. Further preclinical data suggests that downregulation of MAP kinase and Akt with STIVARGA® was shown to sensitize metastatic CRC cells to anti-EGFR therapies, such as ERBITUX®.
The REVERCE trial is a multicenter, randomized phase II trial which enrolled patients with KRAS wild-type metastatic CRC, after failure on combination chemotherapy with Fluoropyrimidine, Oxaliplatin, and Irinotecan. A total of 101 patients were randomized in a 1:1 ratio to receive sequential treatment with STIVARGA® followed by ERBITUX® with or without Irinotecan or reverse sequence of ERBITUX® with or without Irinotecan followed by STIVARGA®. Patients were stratified by prior use of AVASTIN® and intent to use ERBITUX® in combination with Irinotecan. Patients continued each sequence until disease progression or unacceptable toxicity, at which time patients switched to the alternative drug. The Primary endpoint was Overall Survival. Secondary endpoints included Progression Free Survival (PFS) with initial treatment (PFS1), PFS with second treatment (PFS2), Time to sequential Treatment Failure (TTF), Response Rate, Safety, and Quality of Life (QOL). The authors further investigated possible biomarkers including oncogenic mutations from circulating cell free DNA by liquid biopsy, with serial measurements.
It was noted that giving STIVARGA® before ERBITUX® resulted in a significantly longer median Overall Survival of 17.4 months, compared with 11.6 months with ERBITUX® followed by STIVARGA®. After a median follow up of 29 months, there was a 39% reduction in the risk of death with the STIVARGA®-ERBITUX® sequence (HR=0.61; P=0.029). The benefit with STIVARGA®-ERBITUX® sequence was consistently noted across all patient subgroups. In the subgroup of patients with left-sided primary tumors (N=81), patients who started treatment with STIVARGA® first followed by ERBITUX®, had a median Overall Survival of 20.5 months compared with 11.9 months for those receiving ERBITUX® first, and this meant a 49% reduction in mortality risk, which was statistically significant (P=0.01).
The first Progression Free Survival (PFS1) did not differ significantly according to the drug sequence, but the second PFS (PFS2) was more prolonged in those receiving ERBITUX® after STIVARGA®, with a 71% reduction in the risk of progression or death following the second treatment (HR=0.29; P<0.0001). The time to treatment failure was a median of 7.4 months with STIVARGA® followed by ERBITUX® and 6.1 months with ERBITUX® followed by STIVARGA® (HR=0.60; P=0.017). Safety and quality of life were comparable between the two treatment groups.
It was concluded that data from this study suggest that treatment with STIVARGA® first, followed by ERBITUX® resulted in longer survival than that of the current standard sequence and the longer Progression Free Survival following the second treatment period with ERBITUX® may have contributed to the improvement in Overall Survival with the STIVARGA®-ERBITUX® sequence. A biomarker analysis is still ongoing. Randomized phase II study of regorafenib followed by cetuximab versus reverse sequence for wild-type KRAS metastatic colorectal cancer previously treated with fluoropyrimidine, oxaliplatin, and irinotecan (REVERCE). Shitara K, Yamanaka T, Denda T, et al. DOI: 10.1200/JCO.2018.36.4_suppl.557 Journal of Clinical Oncology 36, no. 4_suppl (February 2018) 557-557.
Germline Testing with NGS Multigene Cancer Panels Recommended for All Young Patients with Colorectal Cancer
SUMMARY: ColoRectal Cancer (CRC) is the third most common cancer diagnosed in both men and women in the United States. The American Cancer Society estimates that approximately 140,250 new cases of CRC will be diagnosed in the United States in 2018 and about 50,630 patients are expected to die of the disease. The lifetime risk of developing CRC is about 1 in 21 (4.7%).
Even though the incidence of Colorectal cancer (CRC) in the United States has been rapidly declining overall, primarily driven by screening, the incidence however has been increasing among adults younger than age 50 years. Currently, genetic testing is recommended in patients with polyposis phenotypes, strong family histories, and those whose tumors demonstrate MicroSatellite Instability (MSI) or fail to stain for MisMatch Repair (MMR) gene proteins by immunohistochemistry. Whether patients younger than 50 years of age with CRC, should be tested with a broad multigene panel to detect additional genetic abnormalities, has remained unclear.
The authors conducted this study to ascertain the proportion of young CRC cases associated with genetic predisposition. In this retrospective study, 430 individuals diagnosed with CRC at an age younger than 50 years were evaluated by the clinical genetics service at a single tertiary care cancer center from 1998 through 2015. Data collection included patient histories, tumor phenotypes, and results of germline DNA sequencing. If information was uninformative, germline DNA samples were resequenced using a research-based Next-Generation Sequencing multigene panel. The primary outcome was identification of a pathogenic germline mutation associated with cancer predisposition.
The researchers noted that 26% of young CRC cases had a first-degree relative with CRC and 10% had tumors with histologic evidence for MisMatch Repair (MMR) deficiency and 6% had polyposis phenotype. Germline mutations associated with a hereditary cancer syndrome were identified in 79 patients (18%) following clinically driven germline sequencing, and Next-Generation Sequence analysis using a multigene panel detected actionable germline variants in 6 patients (5%) with uninformative clinical evaluations. Lynch syndrome was identified in 56 patients (14%) of the entire cohort, Familial Adenomatous Polyposis in 2%, MUTYH in 2%, and SMAD4 was mutated in 2 patients, BRCA1 in one, TP53 in one, and CHEK2 in one. Only 51% of the patients with germline mutations associated with a hereditary cancer syndrome gave a family history of CRC diagnosis in a first-degree relative.
The authors concluded that 20% of patients diagnosed with CRC at age younger than 50 years carry a germline mutation associated with cancer, and half of these patients do not have clinical histories typically associated with the identified syndrome. Germline testing with Next-Generation Sequencing multigene cancer panels should therefore be considered for all young patients with CRC. Germline Genetic Features of Young Individuals with Colorectal Cancer. Stoffel EM, Koeppe E, Everett J, et al. Gastroenterology 2017 Nov 13; [e-pub]. (http://dx.doi.org/10.1053/j.gastro.2017.11.004)
OPDIVO® and YERVOY® Combination Improves Survival in Metastatic Colorectal Cancer
SUMMARY: ColoRectal Cancer (CRC) is the third most common cancer diagnosed in both men and women in the United States. The American Cancer Society estimates that approximately 140,250 new cases of CRC will be diagnosed in the United States in 2018 and about 50,630 patients are expected to die of the disease. The lifetime risk of developing CRC is about 1 in 21 (4.7%).
The DNA MisMatchRepair (MMR) system is responsible for molecular surveillance and works as an editing tool that identifies errors within the microsatellite regions of DNA and removes them. Defective MMR system leads to MSI (Micro Satellite Instability) and hypermutation, triggering an enhanced antitumor immune response. MSI (Micro Satellite Instability) is therefore a hallmark of defective/deficient DNA MisMatchRepair (dMMR) system and occurs in 15% of all colorectal cancers. Defective MisMatchRepair can be a sporadic or heritable event. Approximately 65% of the MSI tumors are sporadic and when sporadic, the DNA MisMatchRepair gene is MLH1. Defective MisMatchRepair can also manifest as a germline mutation occurring in 1 of the 4 MisMatchRepair genes which include MLH1, MSH2, MSH6, PMS2. This produces Lynch Syndrome (Hereditary Nonpolyposis Colorectal Carcinoma – HNPCC), an Autosomal Dominant disorder and is the most common form of hereditary colon cancer, accounting for 35% of the MSI colorectal cancers. MSI tumors tend to have better outcomes and this has been attributed to the abundance of tumor infiltrating lymphocytes in these tumors from increase immunogenicity. These tumors therefore are susceptible to PD-1 blockade with immune checkpoint inhibitors.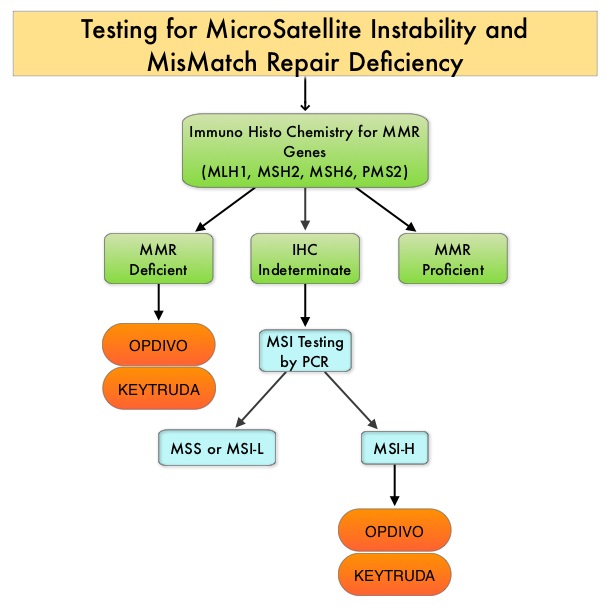
MSI (Micro Satellite Instability) testing is performed using a PCR based assay and MSI-High refers to instability at 2 or more of the 5 mononucleotide repeat markers and MSI-Low refers to instability at 1 of the 5 markers. Patients are considered Micro Satellite Stable (MSS) if no instability occurs. MSI-L and MSS are grouped together because MSI-L tumors are uncommon and behave similar to MSS tumors. Tumors considered MSI-H have deficiency of one or more of the DNA MisMatchRepair genes. MMR gene deficiency can be detected by ImmunoHistoChemistry (IHC). MLH1 gene is often lost in association with PMS2. NCCN Guidelines recommend MMR or MSI testing for all patients with a history of Colon or Rectal cancer.
CheckMate 142 is a large, multi-center, open label, phase II trial which evaluated the efficacy and safety of PD-1 inhibitor treatment in patients with dMMR/MSI-H metastatic colorectal cancer. This study evaluated the benefit of OPDIVO® alone or in combination YERVOY® in this patient population. The rationale behind combining OPDIVO® a PD-1 inhibitor and YERVOY®, a CTLA-4 inhibitor, was based on the synergy between these two agents, to promote T-cell antitumor activity, thereby improving upon single-agent activity of OPDIVO®. The study enrolled 119 patients who received OPDIVO® as a single agent at 3 mg/kg IV every 2 weeks or OPDIVO® 3 mg/kg plus YERVOY® 1 mg/kg every 3 weeks for 4 doses, followed by OPDIVO® 3 mg/kg every 2 weeks. Treatment was continued until disease progression or unacceptable toxicities. The Primary endpoint was Objective Response Rate (ORR) and exploratory endpoints included Safety, Progression Free Survival (PFS), Overall Survival (OS) and efficacy in biomarker-defined populations. This study was not designed to compare the outcomes in these two treatment cohorts. Based on initial data from CheckMate-142, the FDA in July 2017 granted accelerated approval to OPDIVO® for the treatment of patients with MisMatch Repair deficient (dMMR) and MicroSatellite Instability-High (MSI-H) metastatic CRC, that has progressed, following treatment with a Fluoropyrimidine, Oxaliplatin, and Irinotecan.
This review provides an update on outcomes with monotherapy and immunotherapy combination. In the OPDIVO® monotherapy group which included 74 patients, the updated analysis at 21 months showed a response rate was 34%, with 9% being complete responses, and the disease control rate was 62%. The median duration of response has not been reached in the overall cohort of patients and among those responding, 64% had responses lasting at least 1 year. Longer follow up resulted in deepening response rates. The median Progression Free Survival (PFS) for the entire cohort was 6.6 months. Clinical Benefit was seen regardless of PD-L1 expression, BRAF mutation status, KRAS mutation status, and clinical history of Lynch Syndrome.
In the combination immunotherapy group, the median follow up was 13.4 months and the authors of this analysis, André, et al., compared the results of this cohort with those of the OPDIVO® monotherapy group, for the same 13.4 month median follow up period. The most common prior therapies included Fluoropyrimidine (99%), Oxaliplatin (93%) and Irinotecan (73%). Of the 119 patients who received this combination immunotherapy, 76% had 2 or more prior lines of therapy. The Objective Response Rate with a combination of OPDIVO® and YERVOY® was 55%, with 3.4% Complete Responses, and the Disease Control Rate was 80%. About 78% of the patients had reduction in tumor burden with combination immunotherapy. The median time to response was 2.8 months and the median Duration of Response has not yet been reached. Among patients who responded to the combination, 94% had ongoing responses at the time of data cutoff and 63% of the cohort receiving combination immunotherapy remained on treatment. These responses were noted regardless of PD-L1 expression, BRAF or KRAS mutation status, or clinical history of Lynch syndrome. The PFS and Overall Survival with combination immune checkpoint inhibitor therapy at 12 months were 71% and 85%, respectively. There were statistically significant and clinically meaningful improvements in quality-of-life measurements as well.
These data from the CheckMate-142 study support the use of OPDIVO® as a single agent or in combination with YERVOY®, for the treatment of patients with previously treated DNA MisMatch Repair-Deficient/MicroSatellite Instability-High (MSI-H) metastatic CRC.
1. Overman MJ, Bergamo F, McDermott RS, et al. Nivolumab in patients with DNA mismatch repair-deficient/microsatellite instability-high (dMMR/MSI-H) metastatic colorectal cancer (mCRC): Long-term survival according to prior line of treatment from CheckMate-142. Overman MJ, Bergamo F, McDermott RS, et al. J Clin Oncol 36, 2018 (suppl 4S; abstr 554)
2. Nivolumab + ipilimumab combination in patients with DNA mismatch repair-deficient/microsatellite instability-high (dMMR/MSI-H) metastatic colorectal cancer (mCRC): First report of the full cohort from CheckMate-142. André T, Lonardi S, Wong M, et al. J Clin Oncol 36, 2018 (suppl 4S; abstr 553)
